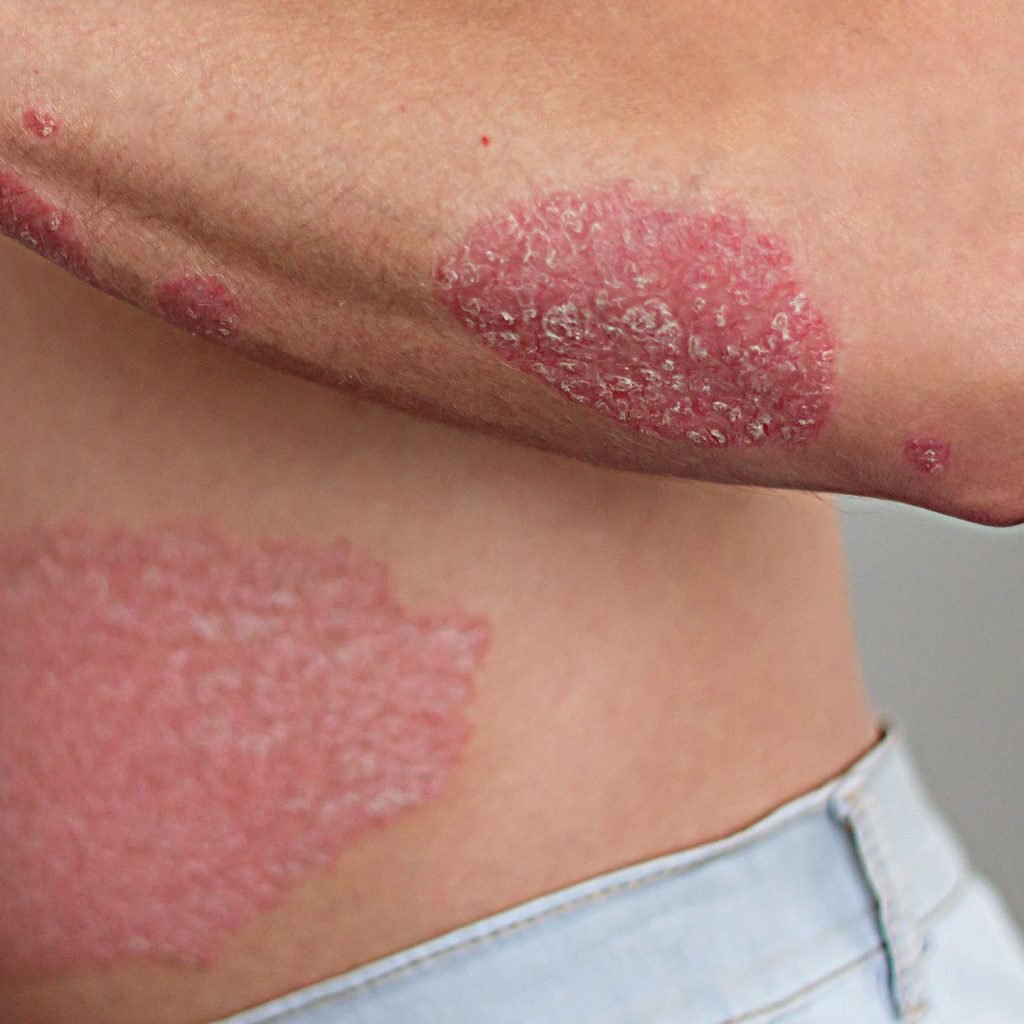
Psoriasis is a chronic autoimmune skin condition that causes red, inflamed, scaly patches on the skin.
It is caused by an overproduction of skin cells that accumulate on the surface of the skin, resulting in patches of raised, red skin with silvery scales.
It can affect any part of your body, but most commonly affects your arms, legs, scalp and back. In some cases, it can also affect your nails, joints and even your genitals.
Symptoms can vary from mild to severe, and can include itching, burning and pain.
Treatment for psoriasis mostly involves topical medications and light therapy, although oral medications can also be used.
Though psoriasis is not contagious, it cannot be cured, but it can be managed with proper treatment.
Psoriasis has different types, and each with symptoms of its own.
Plaque psoriasis: This is the most common, characterised by raised, red, scaly patches your the skin.
Guttate psoriasis: This type is characterised by small, red spots on your skin. It usually impacts children and young adults.
Inverse psoriasis: This type is characterised by bright red lesions in areas of your body where skin folds, such as your armpits and groin.
Pustular psoriasis: This type is characterised by white pustules surrounded by red skin.
Erythrodermic psoriasis: This is a severe form of psoriasis that affects large areas of your body and can cause intense itching, burning and pain.
While it is not life-threatening, it can have serious complications if it is not treated properly.
The most common complication of psoriasis is an increased risk of developing certain medical conditions, such as heart disease, obesity, high cholesterol, stroke and diabetes.
It can also cause joint inflammation and stiffness, contributing to difficulty of movement.
Symptoms can vary from person to person, but the most common ones include:
It is caused by a combination of factors, including genetics, environmental triggers and certain medications.
Here is a list of some of the most common causes of psoriasis:
Genetics: Psoriasis can run in families, and certain genetic factors may increase the risk of developing psoriasis. Studies have shown that if one of your parents has psoriasis, you have a 10% chance of developing the condition. If both your parents have psoriasis, the risk goes up to 50%.
Environmental triggers: Exposure to certain substances, such as cigarette smoke and certain chemicals, can trigger flare-ups of psoriasis. Stress and changes in temperature or humidity can also cause flare-ups.
Medications: Certain medications, such as lithium and beta blockers, can cause psoriasis flare-ups in some people.
Infections: Certain infections, such as strep throat, can trigger psoriasis flare-ups in some individuals.
Hormonal changes: Hormonal changes during puberty, pregnancy and menopause can increase the risk of developing psoriasis.
In order to diagnose psoriasis, your doctor will look at your complete medical history and perform a physical exam.
During the exam, the doctor will look for patches of red or silver skin with thick, flaky scales that are usually itchy.
If your doctor suspects psoriasis, he/she may also order a skin biopsy to confirm his/her diagnosis.
Once psoriasis is diagnosed, a treatment plan will come into play to help manage your condition.
The most common treatment for psoriasis is topical medications, which are applied directly to the affected areas. These medications help to reduce inflammation, slow skin cell growth and reduce scaling.
In some cases, phototherapy may also be prescribed. This involves exposure to ultraviolet light, which can help reduce the effects of psoriasis.
For more severe cases, your doctor may prescribe oral medications or injectable biologic drugs. These drugs help you improve your immune system and reduce your inflammation.
There are many topical treatments available that can help manage the condition. These include:
Topical corticosteroids: These are the most commonly used topical treatments for psoriasis. They work by reducing inflammation, itching and scaling. Topical corticosteroids may not work as efficiently as in the beginning, and their prolonged/overuse may thin your skin.
Topical retinoids: These medications are derived from vitamin A and can help reduce inflammation and slow down the growth of skin cells. Not recommended during pregnancy and breastfeeding.
Calcineurin inhibitors: These medications work by suppressing the immune system, which can help reduce inflammation, itching and scaling.
Moisturisers: Moisturisers can help keep the skin hydrated and reduce itching and scaling.
Salicylic acid: This medication helps reduce scaling and can be used in combination with other topical treatments.
Vitamin D analogues: These help with cell turnover and reduce scaling.
Coal tar: It is another common topical therapy that can help slow the growth of skin cells and reduce inflammation. Not advisable during pregnancy and breastfeeding.
If you have a question related to this blog post, write to us here and we will update this post with a response.
Sources: Cleveland Clinic, Mayo Clinic, WebMD (1, 2, 3, 4, 5), PubMed (1, 2), Medical News Today, National Library of Medicine, Healthline.
If you have any more questions, please feel free to write to us at support@nugenomics.in or call us directly at +91 9176655912
You can also visit Here to know more about how we can help you and make your life better.
Customize your health package