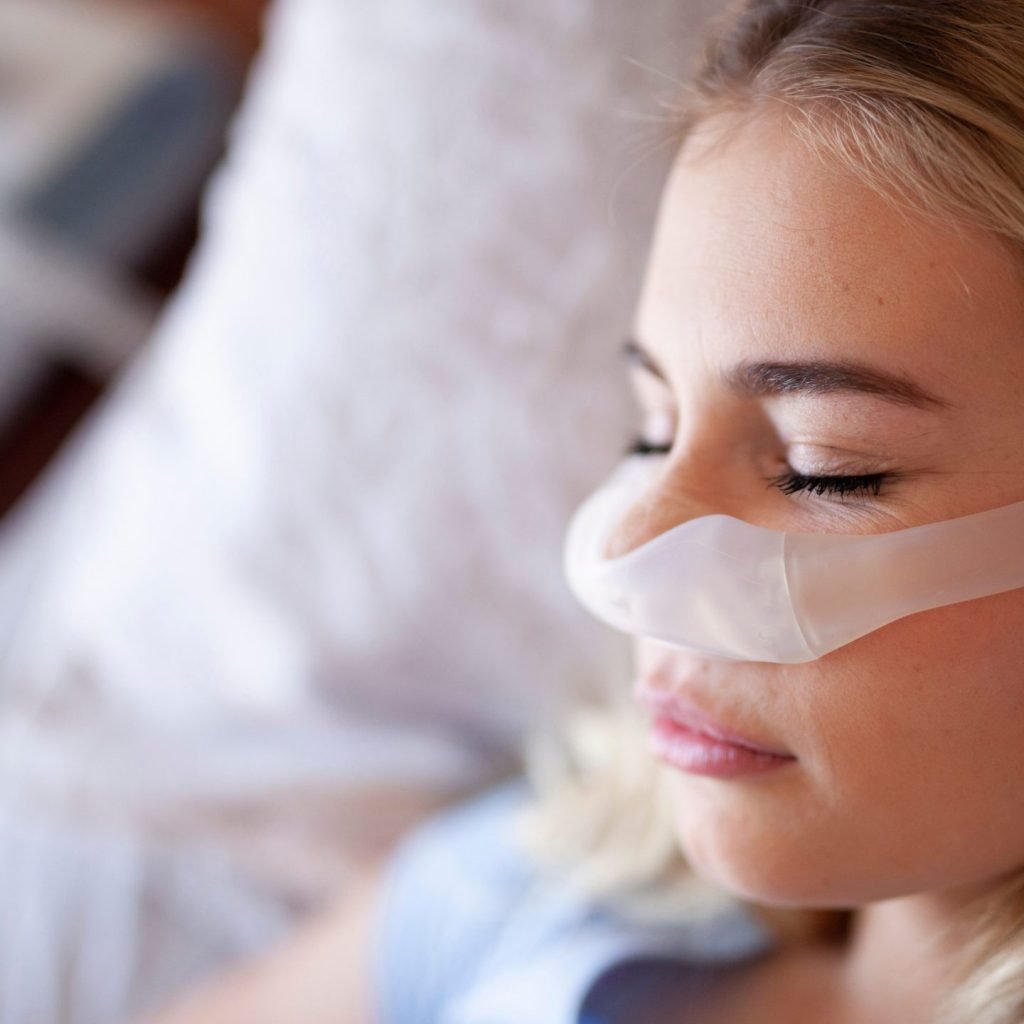
Sleep apnea is a sleep disorder that occurs when your breathing is interrupted during sleep. It is usually caused by an obstruction of your airway, such as when your tongue relaxes and falls back into your throat.
When this happens, you will briefly stop breathing for up to 20 seconds at a time. This can cause you to wake up multiple times during the night, resulting in poor quality sleep and excessive daytime sleepiness.
Sleep apnea can be a serious condition, as it can lead to high blood pressure and heart problems.
Treatment options range from lifestyle changes, such as weight loss and avoiding alcohol, to more drastic measures like surgery or the use of a CPAP machine.
It is the most common type. It’s caused by an obstruction of the upper airway, such as when the tongue falls back and blocks the airway, or when the throat muscles relax too much and block the airway.
Risk factors include obesity, smoking and certain medical conditions.
Treatment typically involves lifestyle changes such as weight loss and avoiding alcohol, along with the use of devices such as CPAP machines to keep the airways open during sleep.
If left untreated, it can increase the risk of heart disease and other health complications.
Central sleep apnea is a type of sleep disorder in which breathing repeatedly starts and stops during sleep. It occurs when the brain fails to send proper signals to the muscles that control breathing.
There are a number of possible causes, including stroke, heart failure and certain medications.
If left untreated, it can lead to serious health complications such as high blood pressure and an increased risk of heart attack and stroke.
Treatment options vary depending on the cause of the disorder, but may include lifestyle changes, medications or CPAP (continuous positive airway pressure) therapy.
Treatment-emergent central sleep apnea refers to a state wherein a patient suffering from OSA undergoes a conversion to CSA after being administered a therapy to treat OSA based on the diagnosis achieved through a sleep study.
In other words, it can develop after the onset of certain treatments, such as opioid analgesics or other medications.
Sleep apnea is a serious condition that can have a major impact on your quality of life, and the sooner it is diagnosed and treated, the better.
So if you’re experiencing any of the following symptoms, promptly talk to your doctor.
Central sleep apnea is caused by an impairment in the brain’s ability to control breathing during sleep.
Obstructive sleep apnea, on the other hand, is caused by physical obstructions to airflow in the upper airways while sleeping, such as the tongue falling back and blocking the airway.
Factors such as age, family history, lifestyle habits, other medical conditions and certain body attributes can increase an individual’s risk of suffering from sleep apnea.
Once the causes are identified, it is possible to take steps to reduce the risks considerably.
It is diagnosed through a series of tests, such as physical examination, sleep study and review of your medical history.
During the physical examination, your doctor will check for signs of sleep apnea, such as snoring and pauses in breathing.
During the sleep study, your doctor will monitor your breathing, heart rate and oxygen levels while you sleep.
The results of the sleep study can help determine if you have the condition.
Additionally, your doctor may ask questions about your medical history and lifestyle to determine if any of these factors could be contributing to your symptoms.
Once diagnosed for sleep apnea, your doctor can recommend treatment options such as lifestyle changes or the use of a continuous positive airway pressure (CPAP) machine.
Nocturnal polysomnography (PSG) is a type of sleep study that is used to diagnose and evaluate sleep disorders.
During the study, multiple physiological activities are monitored, including brain waves, heart rate, breathing, blood oxygen levels and muscle activity. The data from these measurements is used to create a detailed picture of sleep patterns and identify any potential issues.
Nocturnal polysomnography is usually conducted overnight in a sleep lab or hospital setting, and it can take several hours to complete. It is most commonly used to diagnose problems such as insomnia, sleep apnea, narcolepsy and periodic limb movement disorder. This type of sleep study can also be used to evaluate the effectiveness of treatments for specific sleep disorders.
This form of testing enables people to conduct a sleep study from the comfort of their own home. It is similar to an overnight sleep study, though it does not include brain wave monitoring.
This test is not capable of diagnosing central sleep apnea, and is typically not chosen by doctors if they suspect the individual has a more severe form or other sleep-related disorders or medical conditions.
When the home study test does not indicate evidence of sleep apnea, it is usually recommended that the diagnosis be confirmed through an overnight sleep study.
Treatment for sleep apnea may include lifestyle changes such as losing weight, quitting smoking or changing your sleep position.
If you don’t see your improvement in these measures, there are a host of other treatments that can help you.
CPAP is one of the most common and effective treatments for sleep apnea. It involves using a machine to deliver a steady stream of air into your airway while you sleep, helping to keep it open and reduce your apnea episodes.
Oral appliances are custom-made mouthpieces that fit over your teeth and help keep your airway open while you sleep.
Lifestyle changes such as losing weight, quitting smoking and avoiding alcohol before bed can help reduce the symptoms of sleep apnea.
In some cases, surgery may be recommended to treat sleep apnea. This could involve removing tissue from the back of your throat or implanting a device to help keep your airway open.
Unlike traditional CPAP machines, these devices stimulate the nerves in the neck to open the airway so that oxygen can flow freely during sleep. This is done by sending electrical pulses to the hypoglossal nerve, which controls the tongue muscles to keep the airway open.
Studies have shown that these devices can be effective in reducing symptoms of sleep apnea, such as loud snoring, pauses in breathing and excessive daytime fatigue.
Yes, it can.
It is often linked to being overweight, so weight loss is often recommended as a way to reduce the severity of sleep apnea.
A recent study showed that a 10% reduction in body weight led to a 26% reduction in the severity of sleep apnea. This suggests that weight loss can be an effective way to reduce the symptoms of the condition.
If you are overweight and have sleep apnea, speak to your doctor about the best plan for losing your weight.
Generally speaking, the most effective way to lose weight is through a combination of diet and exercise. Eating a healthy, balanced diet and exercising regularly can help you reach a healthy weight and reduce the severity of your condition.
If you have a question related to this blog post, write to us here and we will update this post with a response.
If you have any more questions, please feel free to write to us at support@nugenomics.in or call us directly at +91 9176655912
You can also visit Here to know more about how we can help you and make your life better.
Sources: Mayo Clinic, Cleveland Clinic, WebMD, Medical News Today, NIH, NHS, PubMed, NCBI.

Customize your health package