Type 2 diabetes is a chronic health condition that affects how your body processes insulin.
In people with type 2 diabetes, the body doesn’t produce enough insulin or it doesn’t use the insulin properly, resulting in higher than normal levels of glucose in the blood.
Over time, this can lead to serious health problems such as heart disease, stroke and kidney failure.
Research studies conducted on family twins have demonstrated that genetics are a substantial factor in the development of type 2 diabetes. This is particularly the case considering the influence type 2 has on family history and lineage compared to type 1 diabetes. Furthermore, research has also indicated that race may be a contributing factor.
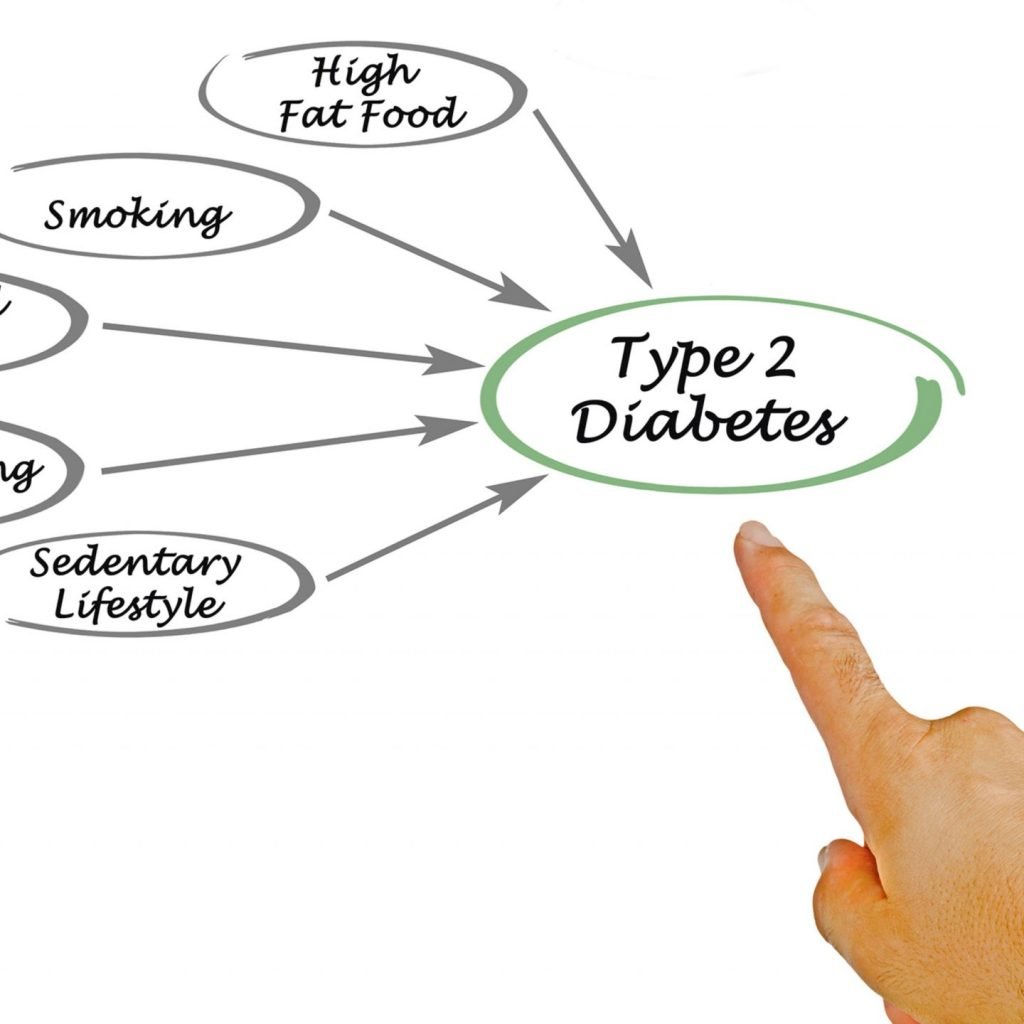
It is also often caused by lifestyle factors such as being overweight or physically inactive.
Type 2 diabetes can often be managed by making lifestyle changes such as eating healthy diet and exercising regularly.
Medication may also be necessary to control blood sugar levels.
For more on diabetes mellitus in general, click here.
You are at risk of developing Type 2 diabetes, if you fall under any of the following:
Type 2 diabetes usually develops over time, and its symptoms may go unnoticed, as they may be less pronounced or mild in the beginning.
Symptoms of type 2 diabetes may include:
If you experience any of these symptoms, talk to your doctor as soon as possible.
Early diagnosis of your condition is a key to effective management or even reversal of your condition.
There is no single cause of type 2 diabetes; rather, it is often the result of a combination of factors that can increase your risk of developing type 2 diabetes. Your body’s resistance to insulin is one of them.
The other causes may include:
Diagnosis of type 2 diabetes is made through a combination of lab tests and medical history. The following tests are commonly used to diagnose type 2 diabetes:
Fasting Blood Glucose Test: A blood test done after an overnight fast to measure the amount of glucose in the blood.
Oral Glucose Tolerance Test: A two-hour test that involves drinking a sweet solution and measuring the amount of glucose in the blood.
A1C Test: A blood test that checks the average level of blood sugar over the past two to three months.
Random Blood Glucose Test: A blood test done at any time regardless of when you last ate to measure the amount of glucose in your blood.
Type 2 diabetes can be managed through lifestyle changes, such as healthy diet and regular physical activity, as well as medications.
The goal of the treatment is to keep blood glucose levels within the target range, reduce symptoms and prevent complications. These include:
Diet and exercise: Eating a healthy diet and getting regular exercise can help reduce blood sugar levels and prevent the development of type 2 diabetes.
Medication: Oral medications such as metformin and insulin injections can help reduce sugar levels in the blood and keep them under control.
Lifestyle changes: Making changes to your lifestyle such as quitting smoking, reducing alcohol consumption and reducing stress can help reduce the risk of developing type 2 diabetes.
Weight loss: Keeping your weight under control help you keep your blood sugar levels within permissible levels.
Please bear in mind that these medications are prescription drugs and must be prescribed by your doctor only. Any attempt to self-medicate is dangerous and will lead to irreversible complications.
For a curated Diabetes Diet Plan, click here. For Superfoods for Diabetes, click here.
The answer to this question is not a simple yes or no. It depends on the type of steroid that is causing the diabetes, as well as the individual’s physiology and health status.
Generally, If you are on steroids, you are at a higher risk of type 2.
Steroid-induced diabetes, also known as steroid-induced hyperglycemia, is a form of diabetes caused by the use of corticosteroids (steroids).
In some cases, the diabetes can be reversed after the steroid use is stopped. However, in some cases, it may last longer than 12 weeks and become permanent.
If this is the case, then you may need to take diabetes medication or insulin injections for the rest of your life.
If you are taking steroids and are concerned about the potential risk for diabetes, it is important to speak to your doctor about your risk factors and the potential for long-term complications.
Your doctor can make recommendations about lifestyle changes or medication adjustments that may help you reduce your risk.
Yes, resistance training can be a very effective tool for managing type 2 diabetes.
Resistance training helps increase your muscle mass, which in turn helps improve your insulin sensitivity and glucose uptake in your body. This can help reduce your blood sugar levels and improve your overall glycemic control.
Also, resistance training has been shown to reduce inflammation, improve good cholesterol levels (HDL) and reduce cardiovascular disease risk, all of which are important for those with type 2 diabetes.
In order to get the most out of resistance training, it is important to work with a knowledgeable trainer who can help you create a program that is tailored to your individual needs.
With the right guidance, resistance training can be a great way to manage type 2 diabetes.
If you have a question related to this blog post, write to us here and we will update this post with a response.
If you have any more questions, please feel free to write to us at support@nugenomics.in or call us directly at +91 9176655912
You can also visit Here to know more about how we can help you and make your life better.
Sources: Mayo Clinic, CDC (1, 2), American Diabetes Association (1, 2, 3), WebMD, NIDDK, Healthline (1, 2), NHS, Cleveland Clinic, SPH, PubMed, NCBI.
Customize your health package